This is the proceeding and slides from a talk I gave at the ABVP Symposium in 2015.
GENERATING EVIDENCE IN PRIVATE PRACTICE
INTRODUCTION
“…the practitioner is an essential part of the total research effort undertaken by our profession and, further, that the barriers between academic and practice life should be lowered so as to integrate the various activities we often designate as “academic”, and practice, research teaching and clinical disciplines.” (Rossdale, 1978)
In a prescient and eloquent article published nearly forty years ago, renowned equine veterinarian Peter Rossdale made the case for encouraging research in private practice. Dr. Rossdale, later an advocate for evidence-based veterinary medicine, recognized the benefits of clinical research in practice to individual veterinarians and the profession as a whole as well as to our patients, who have the most to gain from the production of better research evidence and the development of more effective clinical interventions. The barriers between the domains of research, teaching, and clinical practice, and especially the chasm between academic and private practice, waste talent and resources and retard the production of useful research evidence needed to improve the quality of patient care.
The benefits of conducting research in practice include not only the production of more research evidence but of more clinically relevant and applicable evidence. Clinicians in practice are in the best position to recognize the questions and problems of greatest importance to patient care. While basic research and cutting edge investigations of novel phenomena are ultimately critical to the advancement of medical science, the most pressing and immediate information needs of clinicians often go unmet when those most removed from routine clinical practice set the agenda for research.
Research in practice also has the benefit of improving the scientific literacy of clinicians, giving them greater insight into how the foundational knowledge underlying their clinical practices is produced and what are its limitations. Inappropriate use of diagnostic and therapeutic interventions often stems from a failure to fully understand basic principles of epidemiology, statistics, and other elements of the generation and application of scientific knowledge in medicine. Training clinicians as scientists as well as healthcare providers can improve the depth and sophistication of their understanding of research evidence and how it can be most effectively used to provide optimal patient care.
Integrating research into practice can also have direct personal benefits for practitioners. As Dr. Rossdale put it, “we must provide an outlet for the creative faculties…’students trained in high professional standards may have difficulty in applying these standards to practice.’ And it is this challenge which is recognized by every graduate who turns away from practice, disillusioned by his or her inability to find satisfaction in a situation where the means are not justified by the end that is, where the expectations of training are dashed by the reality of practice.” We can recruit and retain the best minds in veterinary medicine, keep then engaged and motivated, and improve the knowledge base of the profession and the quality of patient by encouraging private practitioners to be researchers and teachers as well as clinicians.
PRODUCING RESEARCH EVIDENCE IN PRACTICE
While the current barriers between academic and private practice, and the paucity of research activities among clinicians outside academia, are unnecessary impediments to the production of more and better research evidence, it is true that some differences between these domains are intrinsic and inevitable. The tangible and intellectual resources available in large institutions with access to large patient populations and those clients most motivated to participate in research do allow academics to engage in types of research activity not practical for clinicians in private practice. Studies requiring expensive equipment, specialized expertise and input from researchers outside of veterinary medicine, and either large numbers of patients or patients with rare diseases, cannot realistically be designed and conducted exclusively in private practice.
Private practice veterinarians could still participate in such studies, as physicians often do, under the auspices of projects coordinated and managed by academic institutions or private industry with the necessary resources. If such distributed, multi-center trials were more common and involved patients in primary or private specialty practice, the amount and applicability of the evidence produced would be improved. This could be a practical method of producing research evidence if a sufficient initial investment were made in setting up networks of practices with appropriately trained clinicians coordinated and supported by academic or industry researchers.
However, there are a number of types of useful research evidence that can be produced in private practice with minimal support from research specialists. These vary in how difficult or costly they are to produce, and how much training and research expertise is required of clinician-researchers. And all good quality research conducted in practice does require clinicians to be familiar with the methodological features of the type of research evidence they wish to generate in order to ensure useful and reliable results with minimal bias. The necessary knowledge and skills can be obtained independently from existing resources, but research in practice could be greatly facilitated by more resources and support from academic researchers and better training of veterinary students in the importance of research and evidence-based medicine methods to high-quality clinical practice.
Clinical Audit
Arguably, clinical audit is not really a type of research in that it is not intended to generate new knowledge but to evaluate the effectiveness of clinical practices in a particular setting relative to other settings or to some accepted standard. However, clinical audit generates important information about the success and limitations of practices in a specific setting, which is necessary in identifying important research questions and areas worthy of investigation. It can also be a simple way of generating observations that can stimulate hypothesis generation or the development of clinical questions for future research. And it provides an opportunity to learn about standardized data collection and to set up mechanisms for collecting and handling data that can also be used for original research.
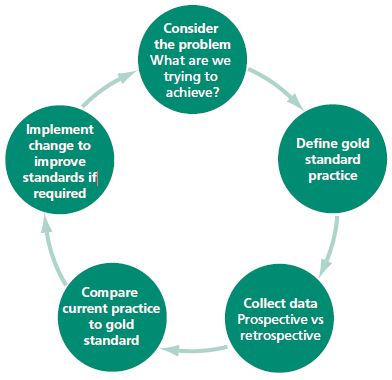
In brief, clinical audit is typically a cyclical process in which one identifies a practice to evaluate and a standard of comparison for the practice, then collects data prospectively or retrospectively to determine the difference between the practice as implemented and the standard. (Figure 1) If necessary, changes are made following analysis of the result and future repetitions of the audit cycle are conducted to assess improvement.
Figure 1. The process of clinical audit (from Dunn, 2012)
The clinical audit process can be used to assess the success or failure of therapeutic interventions or the degree to which the implementation of specific practices are consistent with recommended standards or guidelines. In my practice, for example, we implemented the RECOVER guidelines for small animal CPR (Fletcher, 2012) and then conducted a clinical audit to compare out rates of return of spontaneous circulation and survival to discharge with those reported in the literature. We then reported these data as an example of the impact of the implementation of a clinical practice guideline on outcomes in a private practice, thus adding to the relevant evidence base. (Yagi, 2014)
In veterinary medicine, there will often be no clear gold standard against which to compare the results of audit findings. However, the findings themselves can be useful data not only within the practice but to other clinicians. The results of clinical audits can help in the development of practice standards by showing us where we are now, and they can help identify clinical problems for which controlled prospective research evidence is needed. Clinical audit can also provide clinicians with insight into their own information needs and deficiencies, and with knowledge and experience needed to engage in other research activities. Most importantly, of course, such audits improve patient care.
Case Reports/Series
The type of research evidence private practice clinicians have traditionally bene most likely to produce is the case report or case series. These are descriptions of individual cases or groups of cases with the same clinical problem or subject to the same intervention. Since there are no controls for bias or other sources of error, these reports are appropriate only for suggesting hypotheses to be investigated through controlled research. Case reports and series are low-level, unreliable evidence and should only be used to guide clinical practice with great caution and in the absence of any better quality evidence.
However, such reports are relatively easy to produce, and they provide valuable information about new and uncommon clinical problems or interventions.
Observational Studies
Observational studies do typically involve comparisons among groups of patients subject to different treatments or exposures related to health conditions. They are stronger evidence than uncontrolled case series, but they do not allow for randomization or other important bias control methods, so the conclusions of such studies must still be viewed with some caution and skepticism.
Observational studies can vary from relative simple retrospective analysis of information already collected to complex prospective study designs. Even relatively simple studies assessing the incidence or prevalence of particular health conditions, for example, would contribute significantly to filling information gaps in veterinary medicine. More complex study designs can also generate information about causal relationships between exposures and disease or interventions and outcomes.
Observational studies have particular appeal in private practice because they do not require deliberate, random assignment of subjects to treatment and control groups and the use of placebo treatments, which many clients might be reluctant to consent to. They are often simpler and less costly to conduct than interventional studies, but training and expertise in the relevant research methods is still essential to ensure effective design and execution of observational studies and the production of reliable, useful information.
The development of electronic medical records systems (EMR) has facilitated observational research in human medicine by simplifying the collection and retrieval of data. Properly designed EMR systems in veterinary medicine would make many types of observational research economically logistically feasible for private practice clinicians. Such systems are rare today. However, there are a number of veterinary EMR providers and a fair degree of competition among them, and it is possible that if the capacity to easily collect data and configure such systems for research purposes were widely demanded, manufacturers might be willing to provide these features.
“We are all academics in that we subscribe by our training and our aspirations to scientific objectivity; we are all teachers in that we are anxious to impart our knowledge and wisdom to our colleagues and our successors; we are all practitioners of the veterinary art in one form or another. And each of us have a vested interest in research.” (Rossdale, 1978)
REFERENCES
Dunn, J. Clinical audit: A tool in defense of clinical standards. In Practice. 2012;34:167-169.
Fletcher, D. et al. RECOVER evidence and knowledge gap analysis on veterinary CPR.
Part 7: Clinical guidelines. J Vet Emerg Crit Care. 2012; 22(S1):S102–S131.
Rossdale, PD. Combining research with veterinary practice. Can Vet. J. 1978;19(12):327-330.
Yagi, K. (2014 September ) How RECOVER changed us. International Veterinary Emergency and Critical Care Symposium, Indianapolis, IN.