A key focus of this blog is to promote a science-based perspective for veterinary medicine. I believe that relying more on science and less on habit, tradition, intuition, and personal experience will lead to better care for our patients. While almost everyone claims to support science when asked, it is clear from the topics I report on that many in the veterinary profession, particularly those practicing alternative medicine, don’t really mean it, or at least don’t understand what science-based medicine really means. It is simply impossible to believe in the scientific approach and still practice homeopathy without the most egregious kind of doublethink.
The best hope for improving veterinary medicine and moving further towards science and further away from mysticism and pseudoscience is to teach veterinary students how to think and reason critically, how to evaluate the quality and meaning of different kinds of evidence, and how to recognize and watch out for the errors and biases in their own observation and reasoning; in other words, to teach the epistemology of science and evidence-based medicine.
The alternative, of course, is to teach continuing reliance on blind acceptance of the dogma of one’s teachers and uncritical faith in one’s own observations and the anecdotes of others; in other words, to teach the epistemology of alternative medicine. I have written about the philosophical differences between science and alternative medicine before, and the two often have very different, and incompatible, ways of establishing and verifying knowledge.
Unfortunately, what veterinary students are taught is not determined by any objective standard of reasoning about science and the nature of how knowledge is obtained and evaluated, but by what the teachers believe about the content and processes of veterinary research and practice. And teachers, like all other human beings, have their own biases and interests. There are also complex politics in academia, as in any other human endeavor. And, of course, few of the teachers in veterinary medicine today have themselves been trained in modern evidence-based medicine, which has only become the dominant approach in the human medical profession over the last two or three decades. The practice of passing along the “wisdom of the ages” to the next generation of doctors is far older and more entrenched, however less reliable an approach it may be.
So despite the fact that alternative therapies are currently a relatively marginal part of veterinary medicine, they appear to be growing some in popularity and respectability, and this raises the danger that the next generation of veterinarians will be trained with the idea that even egregious quackery like homeopathy and energy healing are potentially useful practices to be taken seriously. What, then, are the veterinary students of today being taught? How prominent are courses in evidence-based medicine and in alternative medicine?
A thorough answer would require a detailed review of the curricula of all the veterinary schools in the U.S., or any other area one was interested in. I certainly do not have the resources to conduct such a study. However, there is some information available which suggests the relative emphasis on the fields of evidence-based veterinary medicine (EBVM) and complementary and alternative veterinary medicine (CAVM).
The Teaching of EBVM
The Evidence-Based Veterinary Medicine Association (EBVMA) has informally surveyed the veterinary schools in the U.S. and identified which have courses in EBVM and which teach at least some of the methods or concepts of EBVM in other courses. This information is available on the EBVMA web site.
As far as could be determined, of the 35 schools looked at, only one has a course specifically in EBVM, and one other has a course that covers the basics of EBVM along with other material aimed at raising the standard of practice. Beyond that, most schools (26) include some EBVM material in other courses, such as those in public health, epidemiology, and statistics. This suggests that most veterinary students get some exposure to EBVM, but rarely is it presented comprehensively or as an essential strategy for high quality clinical practice.
This is consistent with the findings of a pilot survey, also conducted by the EBVMA in 2011, which suggested most private practitioners have heard some EBVM terms but have little understanding of them and feel unprepared to find and appraise research studies. In this survey, 85% of respondents reported no formal training in literature search and appraisal, and between 30% and 85% were not sufficiently familiar with key EBVM concepts to explain them to others.
It is also consistent with the results of a study carried out in Belgium, in which the decision-making practices of veterinarians were investigated. In that study, “The EBM approach was never mentioned in any of the interviews, with occasional isolated opinions such as ‘The information from research is not important and does not influence decisions.’”
For practicing veterinarians, there is little opportunity to remedy this deficiency in education once they leave school, as there are few courses in EBVM available privately. Some EBVM material is covered in continuing education meetings, and there is a project beginning at one veterinary school to develop EBVM curricula for vets in practice, but the options are limited.
The Teaching of CAVM
A survey of CAVM courses at veterinary schools was conducted in 2011, and it found a somewhat different picture for this collection of therapies.
Sixteen schools indicated that they offered a CAVM course. Nutritional therapy, acupuncture, and rehabilitation or physical therapy were topics most commonly included in the curriculum. One school required a course in CAVM; all other courses were elective… Eighteen veterinary medical schools had no course offerings in CAVM…
4 [schools] had positions (< 0.5 full-time equivalent faculty) devoted to teaching CAVM…
This suggests that CAVM is being taught pretty widely in veterinary schools; perhaps more widely than EBVM. However, CAVM is a heterogenous category notoriously difficult to define. It is common for CAVM proponents to label perfectly ordinary conventional subjects, such as nutrition, as alternative. The inclusion of nutrition in this survey raises questions about whether the therapies being taught were truly alternative (such as raw diets, TCM-guided nutrition, etc.), or simply an appropriation of science-based nutritional recommendations to the standard of “alternative” therapies.
Similarly, physical therapy and rehabilitation are, in human medicine, perfectly ordinary conventional medicine. Due to the limited research in this area in companion animal medicine, this filed is a bit of a gray area at the moment, with reasonable extrapolations from human medicine employed side-by-side with alternative therapies like Veterinary Orthopedic Manipulation, chiropractic, and acupuncture.
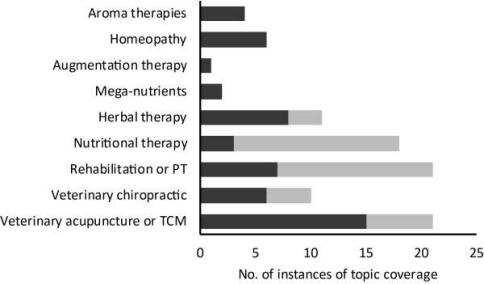
This figure illustrates the sort of CAVM modalities being taught, and it certainly includes both outright quackery, such as homeopathy, and more ambiguous practices.
Figure 1—Coverage of topics in a CAVM course (dark gray bars) or in other courses in the curriculum (light gray bars) at 16 COE-accredited veterinary medical schools that offered a course in CAVM. PT = Physical therapy. TCM = Traditional Chinese medicine.
The survey also suggested that CAVM was more widely taught in 2011 than it had been in a previous survey.
Coverage of CAVM appears to have increased substantially since a previous survey3 of CAVM coverage in veterinary medical curricula. In that survey,3 7 of 23 veterinary medical schools offered courses in CAVM, compared with 16 of 34 schools that offered courses in CAVM in the present survey
It would not surprise me if there has been some growth in the teaching of CAVM as my impression is that there is some growth in the popularity of these therapies in veterinary medicine, though that is difficult to determine objectively. However, the key point regarding the teaching of these methods is made by the authors in this statement:
…the extent of CAVM coverage appears to be driven largely by individual faculty members who happen to have an interest in 1 or more areas of CAVM.
There is no tsunami of new evidence to support greater integration of CAVM in the veterinary curriculum; there are simply individual faculty members interested in such methods. This illustrates the potentially significant impact individual faculty members can have on the profession.
The other key point identified was that the leadership of the veterinary schools appear to have some concerns about the evidentiary integrity of CAVM:
The most frequently and strongly expressed comment in the survey reported here was that any coverage of CAVM in the curriculum, whether in a separate course or as part of other courses, must be via evidence based medicine.
This sounds encouraging, and it indicates that the folks surveyed realize CAVM has a shaky evidence base. However it is unfortunately too easy for proponents of even egregious nonsense like homeopathy to generate the appearance of scientific evidence or rigor. Simple li-service to EBVM or the generation of numerous low-quality studies doesn’t prevent the integration of pseudoscience with CAVM therapies that have real potential benefits.
I have no doubt that the leadership of most veterinary colleges are sincere in their desire that their students be taught truly science-based medicine, I know that the American Holistic Veterinary Medical Association (AHVMA) and other pro-CAVM groups are eager to use research, and funding for research, as a pre-text for promoting therapies that are truly incompatible with legitimate science. The charitable foundation of the AHVMA has made the following statement:
One of our goals is to generate five to seven academic and research teaching hospitals in the United States of America that are qualified, able and willing to do appropriate evidence-based veterinary research into these techniques and philosophies…our ten day campaign that netted over $480,000 in contributions dedicated to this purpose.. Our goal is to generate a twenty million dollar fund to support these centers.
Does anyone believe these individuals or groups will find any CAVM practices to be without merit? Is there any research that can convince the leadership of the Academy of Veterinary Homeopathy that homeopathy is without value? I am not highly confident that the substitution of marketing for real science will be readily seen for what it truly is.
It must also be noted that, in contrast to the situation with EBVM, there are numerous for-profit organizations willing to train and “accredit” veterinarians in the practice of specific CAVM practices. The marketability of alternative therapies is inherently greater than that of the EBVM method, and this makes the financial resources available for promoting and teaching CAVM, and the incentives for doing so, correspondingly greater.
Bottom Line
There is some teaching of the principles and methods of EBVM in veterinary schools, but it is less consistent and integral to the curriculum than it should be, and it is not likely to produce veterinarians committed to EBVM and capable of practicing according to EBVM standards. In contrast, there are much more aggressive and well-financed efforts under way to promote training veterinary students in CAVM methods, both those with some plausibility and reasonable supporting scientific evidence and those that are clearly nonsense. It seems likely that this situation will lead to the greater appearance of legitimacy to CAVM in general, regardless of the actual development of compelling scientific evidence favoring CAVM practices. Students taught CAVM will become vets who practice or refer for CAVM simply because it was presented to them as appropriate in school. Students not taught EBVM will not likely investigate and critically evaluate the evidence base for these practices for themselves but will take the word of their teachers for the value of such therapies. This has the potential to lead to more widespread use of ineffective therapies and less critical thinking among veterinarians, which will not improve the care veterinary patients receive.
It is incumbent, then, upon anyone committed to a sound scientific basis for veterinary medicine that we encourage the teaching of EBVM principles and methods and insist upon the application of these uniformly, to both conventional and alternative practices. No special exemption from scientific standards of evidence should be granted to alternative therapies simply because they have a history of use or dedicated adherents. Truly fair, unbiased, and scientific evaluation of all therapies can only take place if the epistemology of science is accepted as superior to the fuzzy epistemology of history, tradition, and personal experience, and if EBVM methods are consistently, rigorously, and uniformly applied. And this will only happen in the future if veterinary students are trained to think the way now.










Perhaps the problem lies not so much with the education of veterinarians in particular, but with that of the population as a whole. With an adequate grounding in scientific method, and in systems thinking, we would all be far better placed to evaluate the claims of pseudo-science and faith-based assertions. But that would mean growing a population that constantly questioned their elders and betters, and were prepared to use evidence in making decisions, rather than selecting it to justify them after they were made. When I was a young thing, Disgusted of Tunbridge Wells fulminated against rebellious youth and the permissive society, and now I find myself equally furious at thoughtless acceptance and the repressive society!
I think there is definately a connection between the epistemology of the general culture and that of science-based professions. If we were all better trained in critical thinking and less encouraged to accept claims on faith, it would be easier to translate this general approach into an EBVM mindset among veterinarians. Still, science-based professionals are in a category in which opinion-based and faith-based thinking are particularly difficult to justify given the possibility of generatig and using reliable empirical knowledge to answer questions and investigate claims. The standard for such professionals should be higher than for the general populace.
Here’s what we’re up against – including, of course, the enemy of reason within.
http://www.motherjones.com/politics/2013/09/new-study-politics-makes-you-innumerate
I have no doubt that the leadership of most veterinary colleges are sincere in their desire that their students be taught truly science-based medicine, >>>
What’s the scientific evidence for your belief?
Wouldn’t’ the logical conclusion be from their actions rather than their words be they are insincere and do not give a rats ass.
Art Malernee Dvm
I know we often disagree about the intentions of people who practice/promote/tolerate CAM. But there is a difference between factual claims about the physical world and other kinds of beliefs and claims. It is unlikley one could produce relaible, objective scientific evidence about someone’s intentions, so asking for it is really pointless, other than as a snarky rhetorical device. I believe people are most often mistaken about CAM for reasons other than malign intent. You believe otherwise, and we shall have to settle for an unsettled difference of opinion here since there is no objective metric we can appeal to.
“There are in fact two things, science and opinion; the former begets knowledge, the latter ignorance.” ? Hippocrates
Well said, sir!
I have no doubt that the leadership of most veterinary colleges are sincere in their desire that their students be taught truly science-based medicine, >>>>
the Internet is an astonishing invention by which people can access knowledge from anywhere. Back- in -the -day we got together at the local veterinary meeting to fix prices and tell each other it was good medicine because it allowed us focus on quality not cost. We told each other at the meetings that pets do not really need annual vaccines every year but it was ok because it got the pet into the office every year for an annual check up. The information went from one vets mouth to another. Now with the Internet you can show everyone court cases where the attorney generals finally stepped up and started giving us fines for fixing prices. You can show everyone the book (cvt 11 page 207). A book that we were required to buy at vet school thirty years ago that told us pets do not need vaccines every year but it was ok to do it if it got the pet in for annual check ups. I “believe” history will also show that the reason why vet school administrators promote “alternative” medicine is because we do not want non licensed veterinarians doing animal medicine even if it’s bad medicine. That’s the argument I hear from other vets. Their “desire” is to teach more than just science based medicine but also the mumbo-jumbo talk of alternative medicine so that licensed veterinarians do not loose clients to non vets. The argument against doing this at medical schools has been since refined into the mixing apple pie with cow pie metaphor. The argument for is you want someone licensed treating pets even if it’s quackery and only veterinarians are licensed to treat animals in states like Florida.
As a first year veterinary science student, I find this blog refreshing and clarifying.
I wholeheartedly hope that, over the next several years, I am able to fully comprehend the concept of science-based medicine and that I gain the ability to methodically differentiate reliable, peer-reviewed evidence from low-quality, biased, and irreproducible data. I view the skill of critical analysis of new-found information as crucial in the development of knowledge, as it is only upon reliable information that more reliable information can be based.
Welcome, Dominique! It’s always exciting to see someone just starting on their veterinary career. I’ve come to believe that your real job in the next four years is to learn how to think about science and medicine, how to find and evaluate information, and how to communicate much more than it is how to identify and treat any specific disease. I hope it’s a challenging and enjoyable experience, and if I can help in any way please let me know.
In the meantime, here are some resources and contacts you might find useful:
Evidence-Based Veterinary Medicine Association
Centre for Evidence-Based Veterinary Medicine
Students for Best Evidence
Best Bets for Vets
Testing Treatments-A great online resource about how we figure out if our therapies work or not